Appointments & Pricing
All home visits are £45 This price reflects the convenience of me travelling to you.
All new patient appointments at my clinic are £45 for up to 60 minutes.
Follow-up appointments - within my Clinic are £40 for up to 45 minutes.
Routine nail cutting – £35 for one person or £30 per person if TWO people having the same service one after another. These appointments last up to 30 minutes and are strictly for routine nail trimming only, at my discretion and only apply from the second appointment.
Foot Health check - FREE as part of all appointments
These prices do not include verruca treatment.
Preparing for Your Appointment
- Wash your feet on the day of your appointment ( if you can)
- Remove all nail polish ( including Gel ) any nail with polish or gel left on will not be treated (it ruins my equipment)
- If you are DIABETIC or have BROKEN SKIN please DO NOT SOAK your feet
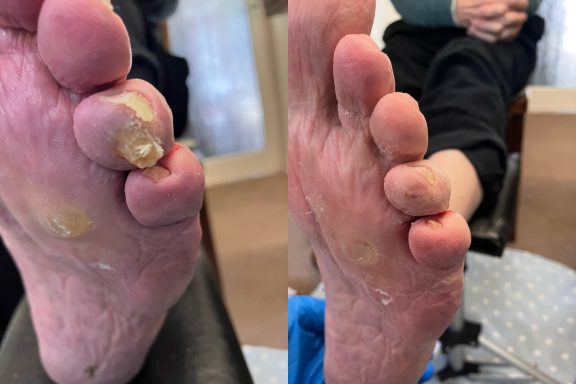
Common foot problems and how they are treated
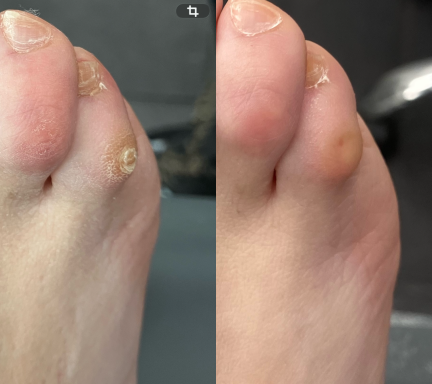
Corns
There are several types of corns, each forming in different areas of the foot and for slightly different reasons.
Hard Corn
A hard corn is a small, concentrated area of thick, hardened skin that usually develops on the top or side of the toes or on areas of the foot that experience pressure from footwear.
Common causes include:
- Tight or poorly fitting shoes
- Toe deformities such as hammer toes or claw toes
- Prominent bones or joints
- High pressure points when walking
How it is treated in the clinic
- Carefully reduce and remove the hard central core to relieve pressure
- Smooth the surrounding skin
- Assess the underlying cause of pressure
- Protective padding or cushioning if needed
- Advice on footwear changes if needed
The treatment is usually quick and provides immediate relief.
What to expect afterwards
After treatment the area may feel immediately more comfortable, particularly when walking. However, corns can return if the pressure that caused them continues.
Soft Corn
Soft corns develop between the toes, most commonly between the fourth and fifth toes. Unlike hard corns, they remain soft because the skin in this area is often moist due to sweat and limited air circulation. They occur when two toes rub together repeatedly, creating pressure and friction between the bones.
Common causes include:
- Tight or narrow footwear
- Toe deformities
- Excessive sweating
- Close toe positioning
Soft corns often appear as whitish or macerated skin and can become very tender due to constant pressure between the toes.
How it is treated in the clinic
- Gently reduce the soft corn to reduce pain and pressure
- Clean and smooth the affected area
- Apply padding or a toe separator to reduce friction
- Advice of footwear if needed
- Silicone toe spaces
- Managing moisture between the toes
What to expect afterwards
Because the toes continue to rub together, soft corns can return without ongoing pressure management.
Seed Corn
Seed corns are small, multiple pinpoint areas of hardened skin that commonly appear on the bottom of the foot, particularly on the ball of the foot or heel. They are usually less painful than other types of corns but may feel rough when walking.
Seed corns develop due to:
- Dry skin
- Repeated friction
- Pressure on the sole of the foot
- Sometimes reduced natural skin oils
They often appear in clusters and look like tiny, hardened plugs in the skin
How it is treated in the clinic
- Carefully remove the seed corns
- Smooth the surrounding skin
- Reduce any thickened callus in the area
- Moisturise the area
- Gel pads or inserts may be advised
What to expect afterwards
After treatment the skin usually feels smoother and more comfortable. Keeping the skin hydrated and managing pressure points helps reduce the chance of seed corns returning.
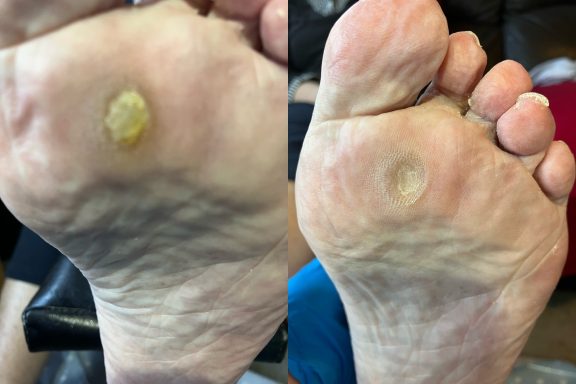
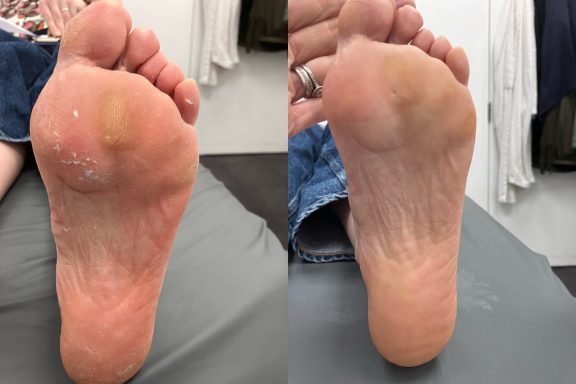
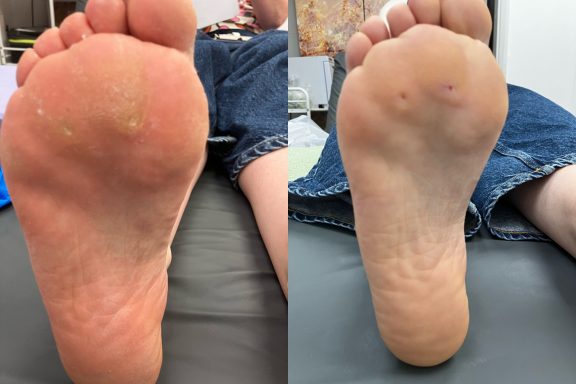
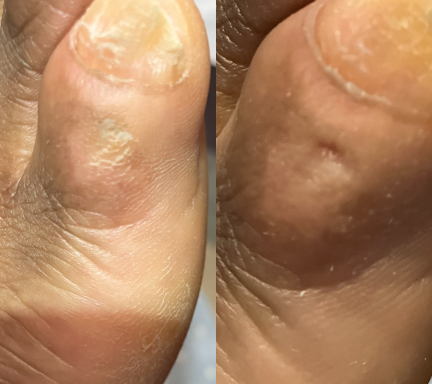
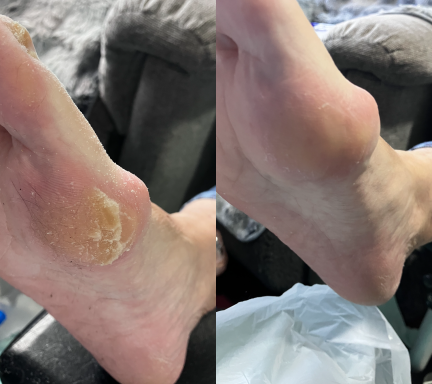
Calluses
Unlike corns, calluses usually cover a broader area and do not have a central core.
A callus is a thickened layer of skin that develops when the body tries to protect an area from repeated pressure or friction. Over time, the skin builds up layers of hardened skin cells which can make the area feel rough, dry and sometimes uncomfortable when walking.
Calluses most often develop on:
- The ball of the foot
- The heel
- The outer edge of the foot
- Areas where bones are prominent
Common causes include:
- Poorly fitting footwear
- High pressure areas when walking or standing
- Foot deformities (such as bunions or hammer toes)
- Abnormal gait or walking patterns
- High activity levels or prolonged standing
While calluses are not usually painful, they can become uncomfortable or cracked if they become too thick.
How it is treated in the clinic
- Carefully reduce the callus
- Smooth the skin to relieve pressure and discomfort
- Assess the underlying cause of the callus formation
- Padding or cushioning to reduce pressure
- Advice on footwear changes
The treatment is quick and usually provides immediate improvement in comfort when walking.
What to expect afterwards
After treatment, the skin should feel smoother and walking may feel more comfortable. However, calluses can gradually return if the pressure on the foot remains. Regular visits to a practitioner may also help keep callus formation under control, particularly for people who are on their feet a lot.
Heel Callus
Heel callus develops when thickened skin forms around the heel due to repeated pressure during walking or standing. This is one of the most common areas for callus formation because the heel absorbs a large amount of body weight. In some cases, the skin can become very dry and may begin to crack, leading to heel fissures.
Common causes include:
- Dry skin
- Open-back footwear (such as sandals)
- Prolonged standing
- Increased body weight
- Reduced natural skin elasticity with age
How it is treated in the clinic
- Reduction of the callus with various methods
- Smoothing the skin surface
- Treating any heel fissures if present
- Applying padding or protective dressings if needed
- Moisturising the area
What to expect afterwards
After treatment the heels often feel significantly smoother and more comfortable. Regular maintenance care may prevent it from becoming excessively thick again.
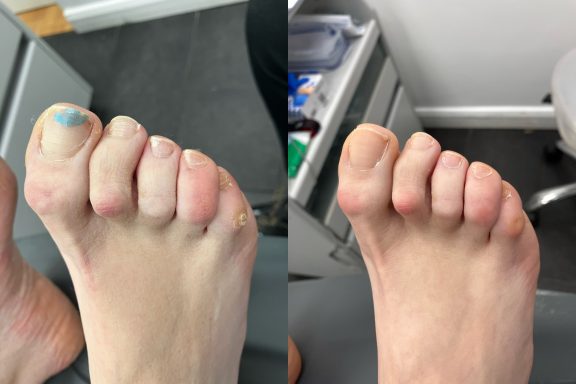
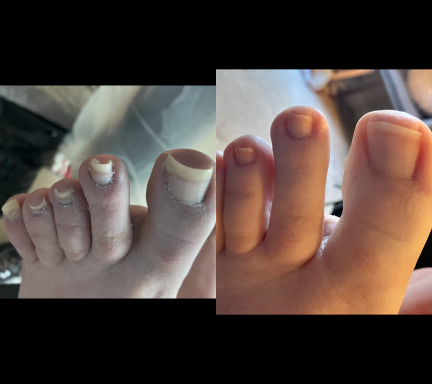
Nail Trimming
Regular professional nail care helps keep the nails comfortable, healthy and reduces the risk of complications such as ingrown nails or nail infections. Some people are unable to safely manage their own toenail care. Nails may become difficult to cut due to several reasons including:
- Thickened or hard nails
- Curved or involuted nails
- Reduced mobility or flexibility
- Poor eyesight
- Arthritis in the hands or hips
- Diabetes or circulation problems
- Difficulty reaching the feet safely
When nails are not trimmed regularly, they can become long, sharp, thick or uncomfortable in footwear. This can sometimes lead to pressure on the surrounding skin or the development of painful nail problems.
Routine professional nail care helps prevent these issues from developing.
How it is treated in the clinic
- Assessment of the nails and surrounding skin
- Safe trimming of the toenails
- Reduction of thickened nail if present
- Filing and smoothing of the nail edges
- Removal of any sharp corners or rough edges
The treatment is gentle, safe and usually takes only a short time to complete.
What to expect afterwards
After treatment the nails should feel smooth and comfortable in footwear. Most patients find walking and wearing shoes more comfortable once the nails have been properly trimmed. For patients who are unable to manage their own nail care, regular appointment of 6-8 weeks are advised to prevent future problems.
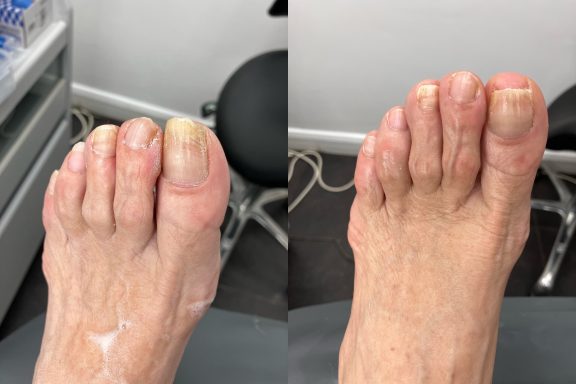
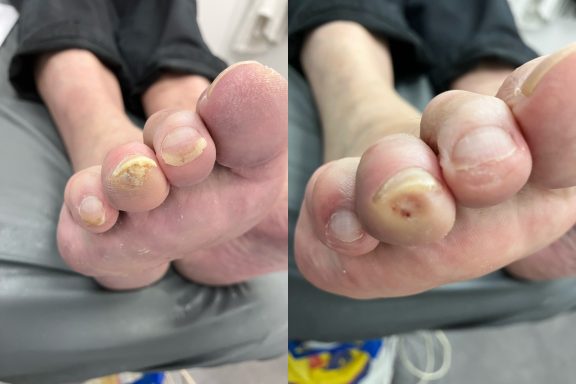
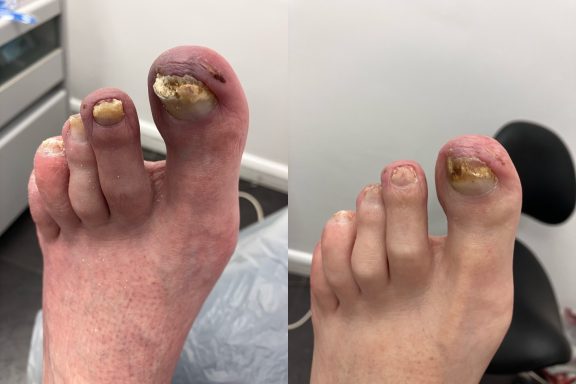
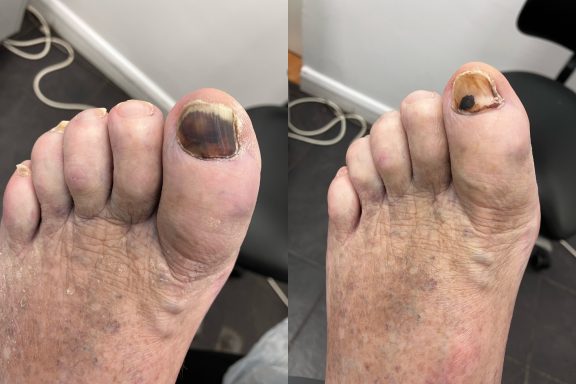
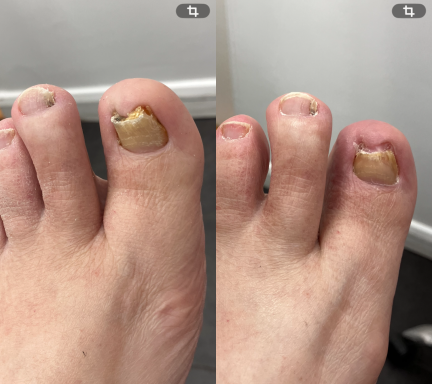
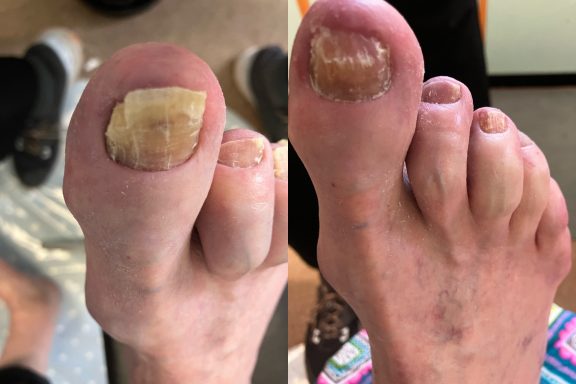
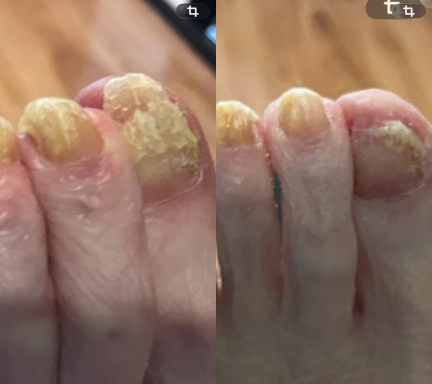
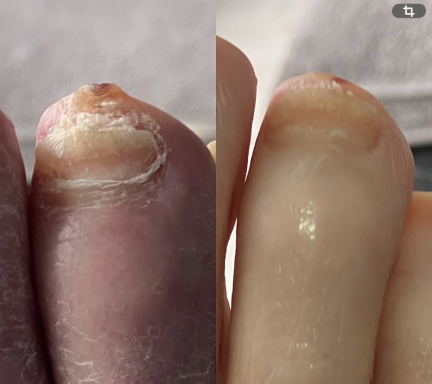
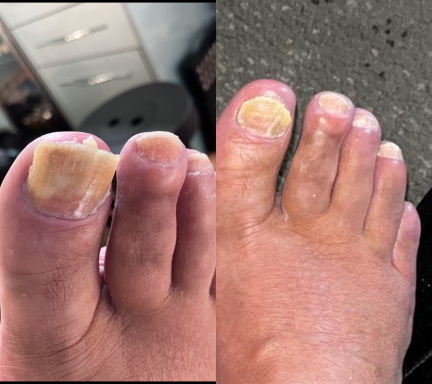
Fungal Nails
Fungal nail infections are a common condition that affects the toenails.
It occurs when microscopic fungi enter the nail through small cracks in the nail or surrounding skin. The fungi then grows slowly within the nail, causing it to become thickened, discoloured and sometimes brittle.
Common signs of fungal nails include:
- Yellow, white or brown discolouration
- Thickened nails
- Crumbly or brittle nail edges
- Nails lifting away from the nail bed
- Distorted nail shape
The infection is more likely to develop in warm, moist environments where fungi thrive.
Common causes and risk factors include:
- Sweaty feet or damp footwear
- Walking barefoot in communal areas such as swimming pools or gyms
- Minor nail injuries
- Athlete’s foot infections spreading to the nail
- Poor circulation
- Diabetes or reduced immune function
Fungal nail infections are not usually painful but can become uncomfortable if the nail becomes very thick.
How it is treated in the clinic
- Professional reduction and thinning of the thickened nail
- Removal of loose or infected nail material from under and around the nail
- Advice on appropriate antifungal treatments
Other options are
- Topical antifungal solutions or lacquers to improve the appearance
- Referral to a GP if the appearance is bothersome to see if an oral antifungal medication is compatible.
Follow-on advice and what to expect afterwards
Fungal nail infections can take time to improve because toenails grow slowly. It may take several months for a healthy nail to fully grow out. Regular nail reduction can help make the nail more comfortable and improve the effectiveness of antifungal treatments. With the right care and treatment, the appearance of the nail may gradually improve as new healthy nail grows.
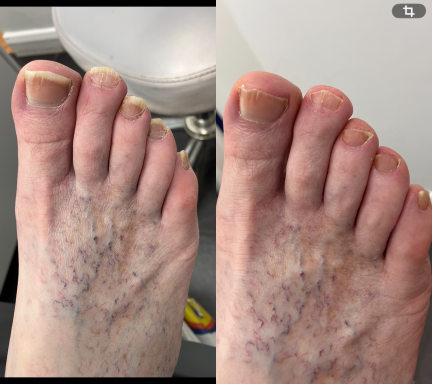
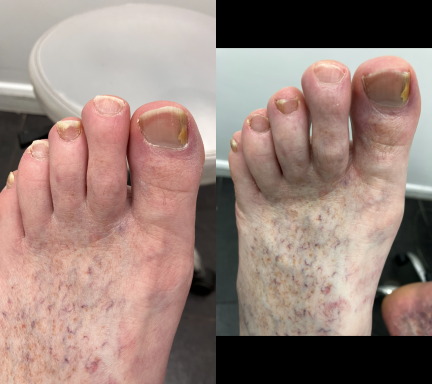
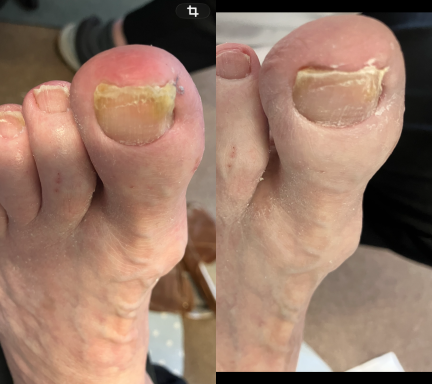
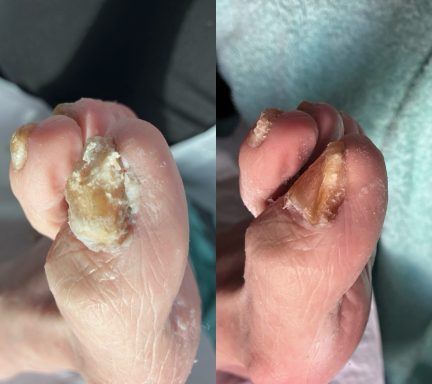
Thickened Toenails
Thickened toenails occur when the nail plate gradually becomes thicker over time. This can happen for several reasons and may develop slowly without being noticed at first.
- Nails that are difficult to cut
- Yellow or opaque appearance
- Nails becoming raised or bulky
- Rough or uneven nail surface
- Pressure or discomfort in shoes
There are several possible causes of thickened nails, including:
- Repeated trauma or pressure from footwear
- Previous nail injury
- Age-related changes to the nail
- Long-standing fungal nail infection
- Reduced circulation
- Certain skin conditions
Over time the nail may become increasingly hard and difficult to manage without professional care.
How it is treated in the clinic
- Carefully reduce the thickness of the nail
- Trim and reshape the nail
- Smooth the nail surface to reduce pressure in footwear
- Assess the nail for signs of fungal infection or other conditions
Regular nail reduction appointments are often recommended to keep the nail comfortable and manageable.
What to expect afterwards
After treatment the nail will usually feel much thinner and more comfortable in footwear. Because the underlying cause may still be present, the nail can gradually thicken again over time. Routine clinic appointments can help maintain the thickness.
Ingrown Toenails
A true ingrown toenail develops when the side or corner of the nail presses into or grows into the skin next to the nail. This causes irritation and inflammation in the surrounding tissue. If the problem continues, the area can become increasingly painful and may develop infection. An ingrown toenail is sometimes mistaken for what is a build-up of skin cells compacted into a tight spot.
Common signs of an ingrown toenail include:
- Pain along the side of the nail
- Redness and swelling around the nail
- Tenderness when pressure is applied
- Possible discharge or infection in more advanced cases
Several factors can contribute to ingrown toenails, including:
- Cutting the nails too short or rounding the corners
- Tight or narrow footwear
- Injury to the nail
- Naturally curved nails
- Repeated pressure on the toes
- Excessive sweating
Without treatment the condition may worsen and become increasingly uncomfortable.
How it is treated in the clinic
Treatment depends on the severity of the ingrown toenail. For mild or early cases we may
- Carefully trim and reshape the nail
- Remove the portion of nail causing pressure
- Clean the area and reduce inflammation
For more severe or recurring cases where local pain relief may be required you would be referred to a podiatrist. Treatment could include:
What to expect afterwards
After treatment, most patients experience relief from the pressure and discomfort. The toe may feel slightly tender for a short time, particularly if the nail edge has been removed. Regular appointments can help keep nails healthy and prevent future ingrown nails.
Athlete’s Foot
Athlete’s foot is caused by fungi that infect the outer layer of the skin. These fungi grow particularly well in warm and damp conditions, such as inside shoes and socks. The infection most commonly develops between the toes, where moisture can become trapped.
Common signs and symptoms include:
- Itching or burning between the toes
- Red, inflamed skin
- White, soggy or peeling skin between the toes
- Dry, flaky or cracked skin on the soles of the feet
- An unpleasant foot odour
In some cases, the skin may split or crack, which can become sore or lead to secondary infection.
Common causes and risk factors include:
- Sweaty feet
- Wearing tight or non-breathable footwear
- Walking barefoot in communal areas such as gyms, swimming pools or changing rooms
- Sharing towels or footwear
- Having a weakened immune system
Athlete’s foot can sometimes spread to the toenails if not treated promptly.
How it is treated in the clinic
- Advice on appropriate antifungal creams or sprays
- Cleaning and reducing any thickened or damaged skin
- Guidance on managing moisture and foot hygiene
- Monitoring for any spread of infection to the toenails
What to expect afterwards
With the correct treatment at home, athlete’s foot usually improves within a few weeks.
Verrucae
Verrucae are small viral growths that develop on the skin of the feet. They are caused by the human papillomavirus (HPV) and commonly appear on weight-bearing areas such as the soles of the feet or the heel. Because they occur on the bottom of the foot, pressure from walking can push the verruca inward, sometimes making it uncomfortable.
A verruca develops when a virus infects the outer layer of the skin, usually entering through tiny breaks or damaged skin. The virus causes the skin cells to grow rapidly, forming a small rough lesion on the foot.
Common signs of a verruca include:
- A small rough patch of skin on the sole of the foot
- Tiny black dots within the lesion (small clotted blood vessels)
- Thickened skin around the area
- Discomfort or tenderness when walking or standing
Verrucae are contagious and can spread through direct skin contact or from contaminated surfaces.
Common places where they may spread include:
- Swimming pools
- Changing rooms
- Gym floors
- Communal showers
Children and young adults are more commonly affected, but verrucae can occur at any age.
How it is treated in the clinic
Treatment options may include:
- Careful reduction of the thickened skin covering the verruca
- Application of specialist topical treatments
- Protecting the area if it is painful when walking
In some cases verrucae may resolve naturally over time as the body’s immune system clears the virus.
Treatment aims to reduce discomfort, manage the lesion and help encourage resolution. A topical treatment with Verrutop is an additional £30 per treatment.
What to expect afterwards
Verrucae can sometimes take time to clear and may require several treatments depending on the size and location. Many verrucae will gradually resolve as the immune system clears the virus, although this can take several months. If the verruca becomes painful or spreads, further treatment may be recommended.
Diabetic Foot Care
Why Foot Care Is Important for People with Diabetes
People living with diabetes need to take extra care of their feet. Diabetes can affect both the circulation and the nerves in the feet, which means small problems can sometimes develop into more serious complications if they are not noticed or treated early.
Regular foot care and podiatry checks are an important part of maintaining good foot health and preventing problems.
Why is the connection between Diabetes and the feet.
Diabetes can reduced sensation in the feet, known as diabetic neuropathy. This means that cuts, blisters or pressure areas may not be felt straight away.
Diabetes can also reduce blood circulation, which can slow down healing and make the skin more vulnerable to injury.
Because of these factors, even small problems such as:
- A blister
- A small cut
- A corn or callus
- An ingrown toenail
can potentially develop into more serious issues if they are not managed early. For this reason, regular professional foot checks are strongly recommended for people with diabetes.
How diabetic feet are cared for in the clinic
During a diabetic foot care appointment, a podiatrist will assess the overall health of the feet and look for any early signs of problems.
This may include:
- Checking the skin for cuts, cracks or infections
- Assessing circulation in the feet
- Testing sensation and nerve function
- Safely trimming and caring for the toenails
- Treating corns, callus or other pressure areas
Regular appointments are often recommended to help maintain healthy feet.
Foot care advice for people with diabetes
Good daily foot care is very important for people with diabetes. Some key recommendations include:
Check your feet every day
Look for any redness, cuts, swelling, blisters or changes in the skin or nails.
Avoid walking barefoot
Always wear footwear or slippers to protect the feet from injury.
Do not soak your feet for long periods
Soaking can soften the skin too much and make it more vulnerable to damage.
Keep the skin moisturised
Apply moisturiser to dry skin to prevent cracking, but avoid putting cream between the toes.
Wear properly fitting footwear
Shoes should provide good support and enough space for the toes.
Keep feet clean and dry
Dry carefully between the toes after washing.
Do not attempt to cut corns or calluses yourself
Always seek professional podiatry care.
Looking after your feet is an important part of managing diabetes and maintaining mobility and comfort.